This sample Skin Diseases Research Paper is published for educational and informational purposes only. If you need help writing your assignment, please use our research paper writing service and buy a paper on any topic at affordable price. Also check our tips on how to write a research paper, see the lists of health research paper topics, and browse research paper examples.
Introduction
Noncancerous skin diseases encompass a wide variety of infectious, inflammatory, and autoimmune diseases. Skin is not only unique in being the largest organ in the body, but also the only organ visible to the patient and physician. Hence the disorders of the skin, though sometimes cosmetic, can have psychological implications for the patient. Being a visible organ, the skin and its diseases are amenable to topical therapies that can provide immediate satisfaction to the patient. Since skin type greatly varies across continents, the most common diseases on one continent can be a rarity on another. For example, skin cancer patients form a vast majority of outpatient visits in North America and Australia but are rarely seen in Asian countries. Due to the wide variety of observable diseases, this research paper focuses on the most common dermatological diseases encountered during outpatient visits all over the world.
Acne
The most common type of cutaneous disorder in the world is acne vulgaris. Acne has a high prevalence in adolescents – nearly 85% – and mildly affects adults. The pathophysiology of acne is increased androgen secretion, colonization by Propioniobacterium acnes, and increased sebum production.
Other forms of acne are caused by cosmetics, oils, greases, creams, and dyes. Acne has also been associated with various hormonal states such as pregnancy, adolescence, and even disorders such as polycystic ovary syndrome and SAHA (seborrhea, acne, hirsutism, and androgenetic alopecia) syndrome. Various drugs such as barbiturates, bromides, corticosteroids, and certain vitamins such as B2, B6, and B12 can cause acne.
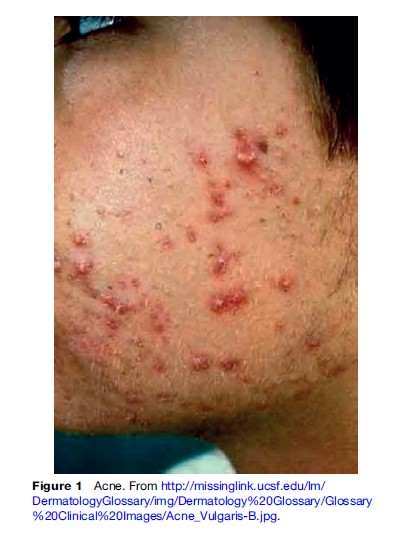
The clinical spectrum of acne ranges from open and closed comedones, papules, pustules, and sometimes cystic acne. It usually affects the face, neck, chest, upper back, and upper arms. Severe acne and certain variants of acne such as acne fulminas and acne conglobata can be painful, distressing, and very difficult to treat. Severe acne can also heal with extensive acne scarring. Acne scarring can have a significant psychological impact on the patient and can be a source of social embarrassment, anxiety, and shame in the patient’s life.
Mild to moderate acne is treated with topical applications of benzyl peroxide, retinoids, and antibiotics. For more severe acne, long courses of antibiotics and retinoids are warranted. Acne scarring can be treated with sometimes expensive surgical interventions such as dermabrasion, microdermabrasion, fillers, and even lasers. Along with the treatment of acne it is crucial to address the social concerns of the patient and treat any associated psychological issues (Figure 1).
Psoriasis
Psoriasis is an inflammatory disorder that affects 0.6%–4.8% of the population worldwide. Psoriasis is an organ-specific autoimmune disorder and is the most prevalent immune-mediated disease in adults. A genetic component increases the susceptibility to psoriasis and the exact etiopathogenesis of psoriasis still needs to be elucidated. Psoriasis is known to be exacerbated by stress and physical injury and can form new lesions at sites of injury, which is known as Koebner’s phenomenon.
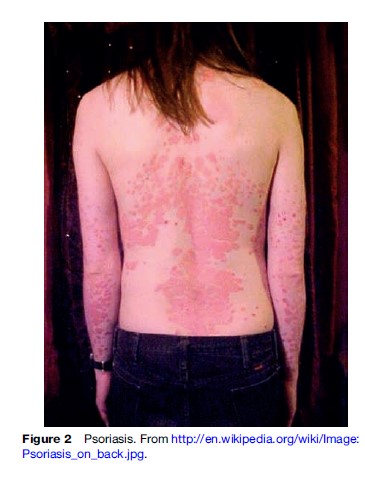
It is commonly characterized by erythematous papules and plaques often topped with a silver scale. The classic involvement is elbows, knees, palms, and soles of the feet. The erythema and scaling attributed to psoriasis are the result of hyper proliferation and atypical differentiation of the epidermal layer, along with inflammation of cell infiltrates and various vascular malformations. It is commonly characterized by erythematous papules and plaques that produce a silver scale.
There are many oral and topical treatments for psoriasis. Inexpensive treatments such as hydration and emollients help keep the skin soft and moist while minimizing the itch and tenderness; petroleum jelly and thick creams are among these treatments. Other treatments include glucocorticoids, which focus on anti-inflammation, ant proliferation, and suppressing the immune response (Figure 2).
Eczema
Eczema (atopic dermatitis) is a chronic inflammatory skin disease. Eczema is caused by genetics and sometimes has allergic features. Chromosomal studies show that eczema is inherited from a maternal gene located on chromosome 11. Eczema affects 8–25% of the population worldwide. This disease occurs in all races and geographic locales; although a higher incidence of eczema is found in urban populations.
The immunological mechanisms of eczema are not completely understood and no marker for the disease has been discovered. Eczema is characterized by reduced cell-mediated immunity, abnormal antibody-dependent cellular cytotoxicity, and high concentrations of serum IgE. People with eczema are far more prone to psoriasis and other diseases that affect the skin barrier. People with eczema are likely to get bacterial or viral infections due to the weak skin barrier.
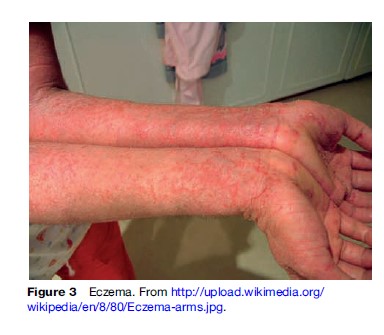
In young children, eczema can appear as acute skin lesions and pruritic erythematous zones with papules. Scaling on the face, scalp, extremities, or trunk have been commonly seen. Treatments of eczema include immune regulation via corticosteroids, UV light therapy, and cyclosporine given orally. Other therapies attack exacerbating factors such as itch and tenderness by the use of emollients and creams. Minimal contact with dust and upholstery reduces exposure to dust mites, reducing the severity of eczema (Figure 3).
Keloids
The word keloid means tumor-like in Greek. The keloid is a benign fibrous growth that presents itself in scar tissue as a result of altered wound healing. In the keloid, extracellular matrix and dermal fibroblasts are overproduced with a high mitotic rate. Exactly how keloids form is not known. Keloids have a high occurrence rate in Blacks and dark-skinned individuals with skin trauma.
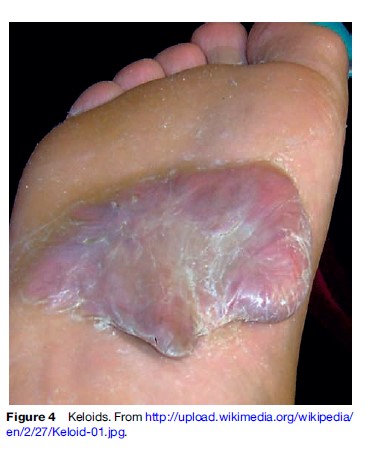
Keloids are characterized by excessive scar tissue and some patients complain of sharp, shooting pains. Keloids commonly appear on the ears, neck, jaw, chest, shoulders, and upper back. They are commonly mistaken for hypertrophic scars.
Prevention is the best treatment for patients with a predisposition to keloidal formation. Excision is another common treatment, along with intralesional corticosteroids or cryosurgery. In many cases, combination therapies are used. The recurrence of keloidal growth is common after treatment (Figure 4).
Rosacea
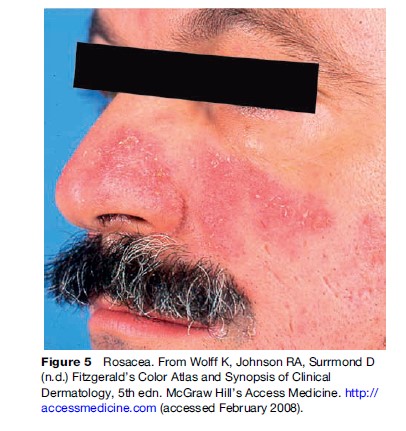
Rosacea is an acne-like disorder that occurs in middle-aged or older adults. Rosacea is characterized by vascular dilation of the central face. Rosacea is a chronic disease that occurs in patients with fair skin and light hair and eye color. The cause of rosacea is unknown.
Currently, there are no specific diagnostic tests to detect rosacea in patients. Some features are seen in most rosacea patients, including flushing (transient erythema), nontransient erythema, papules, pustules, and telangiectasia. Some common symptoms of rosacea are burning or stinging, plaque, dryness, and edema.
For treatment of rosacea, control is the primary goal. Topical antibiotics or benzoyl peroxide are the initial treatments to relieve the inflammatory lesions. For popular or pustular lesions, the following can be applied: metronidazole, azelaic acid, sodium sulfacetamide, and acaricides. For persistent symptoms, tretinoin cream and oral antibiotics are commonly used (Figure 5).
Alopecia Areata
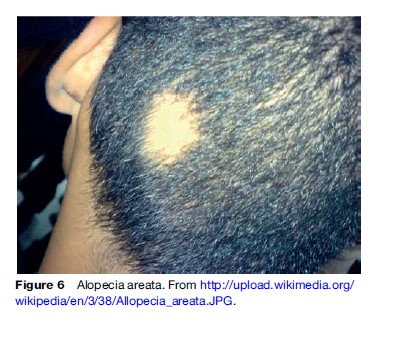
Alopecia areata is a nonscarring inflammatory disorder affecting hair follicles, causing patchy or complete hair loss. The etiology is autoimmune and can be associated with other autoimmune disorders such as vitiligo and thyroiditis. It can affect men, women, and children alike. Though it is noninfectious and noncontagious, its location, chronic nature, and difficulty in treatment can have psychological implications for the patient.
Alopecia areata can cause patchy hair loss on the scalp or beard or involve the entire scalp (alopecia totalis) or also the entire body (alopecia universalis). The characteristic presentation of alopecia areata patches is bald patches that are surrounded by broken off hairs, giving the appearance of exclamation points.
Many patients with alopecia areata can go into spontaneous remission without treatment. Those who require treatment are given topical steroids such as clobetasol and fluocinonide. Moderate success has been achieved with injectable steroids. Topical irritants such as coal tar and anthralin do not have the side effects seen with steroids. Immunomodulators such as cyclosporine have also shown some success in the treatment of recalcitrant alopecia areata. Along with the treatment, it is important to address the significant anxiety and stress the patient may experience (Figure 6).
Vitiligo
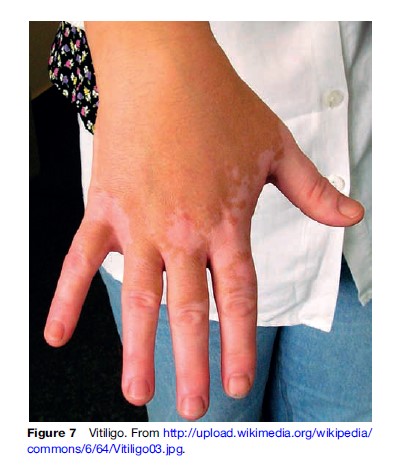
Vitiligo is an acquired disorder of depigmentation of great cosmetic significance. The prevalence of this diseases ranges from 0.1 to 4% in some populations. Generally, patients with darker skin type face great stigmatization due to this disease.
Though the disease is noninfectious, noncontagious and has mostly cosmetic concerns, patients are greatly concerned about the disease because of social attitudes toward the disease. In developing countries, it is quite commonly mistaken to be leprosy, which can be devastating for the affected patient. Because of the autoimmune nature of the disease, it can be associated with other autoimmune disorders such as hyperthyroidism, pernicious anemia, and alopecia areata. The symptoms of the disease are the presence of depigmented (loss of color) patches over parts of the body. The patches can remain localized or may spread to become generalized. Patients do not have itching or pain associated with the patches.
Though there is no universally accepted definitive treatment for vitiligo, various modalities have been tried. Topical applications of corticosteroids, immunomodulators, and topical psoralen have been used. When larger areas of the body are involved, systemic corticosteroids, narrow-band UVB, and psoralen with UVA have shown moderate responses. Surgical treatments include split skin grafting, suction blister grafting, and use of newer lasers. When patients have extensive vitiligo, physicians depigment the remainder of the normal pigment skin using 20% hydroquinone creams to minimize the contrast between pigmented and depigmented skin. Research is ongoing in the field of vitiligo, but importantly, a complete understanding of the benign, noncontagious nature of the disease and adequate support from groups can help patients be in terms with the disease (Figure 7).
Warts
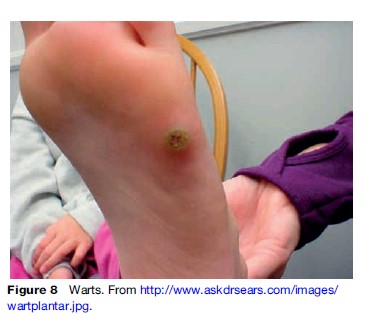
Also called verrucae, cutaneous warts occur when human papillomavirus (HPV) infects epithelial tissue of the skin and mucous membranes. Cutaneous warts commonly occur in children and young adults. Warts can occur singularly or in groups, forming a hyperkeratotic layer to shield itself. HPV infection occurs by skin-to-skin contact. Spontaneous remission of cutaneous warts is common and is seen in up to two-thirds of patients.
Current therapies for cutaneous nongenital warts include debridement accompanied by freezing with liquid nitrogen, treatment with salicylic acid, bichloracetic acid, or cantharidin. Flat warts are treated with cryotherapy, 5-fluorouracil, or tretinoin. While filiform warts are generally treated with a snip excision, imiquimod is a common topical treatment for anogenital warts, working through local cytokine induction. It has been shown that a combination therapy of gentian violet and liquid nitrogen can be used as a less invasive treatment (Figure 8).
Urticaria
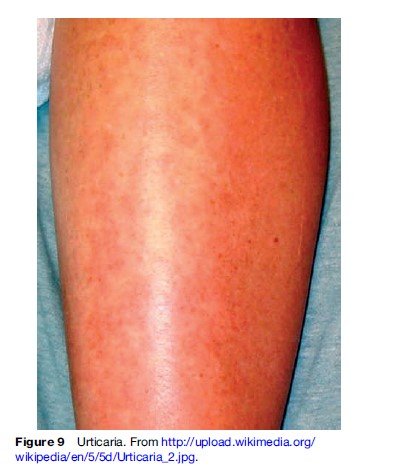
Urticaria, commonly known as hives, is a common disorder described as a lesion that is intensely pruritic, circumscribed, raised, erythematous plaque, often with central pallor. These lesions then typically will disappear over a few hours without leaving residual marks on the skin.
Urticaria is divided into acute or chronic forms depending on the duration of the disease. Urticaria of less than 6 weeks duration is called acute, whereas urticaria lasting more than 6 weeks is chronic. It is caused by histamine release in the skin, which can be an allergic or nonallergic phenomenon. Physical urticaria can be caused by heat, cold, vibration, pressure, etc. Various drugs such as sulfonylureas, aspirin, and penicillin can cause urticaria.
The most challenging but most rewarding task in management of urticaria is to identify the source of the lesions. If the trigger is removed, urticarial lesions will subside. For symptomatic relief, antihistamines such as cetirizine and loratadine are given and can also be used prophylactically. For severe outbreaks, a short course of high doses of corticosteroids can be given (Figure 9).
Pediculosis
The head louse is an adaptable creature that has been able to survive in the advanced societies of the Western world. Children are most commonly affected. Interaction with playmates, cross-transfer from articles of clothing on adjacent hooks in school cloak rooms, and shared combs, headphones, towels, and beds are important modes of disease spread. Hair length is not a factor.
The head louse is a gray-white, active insect, 3–4 mm in length. The female is a little longer than the male. Both sexes are equipped with mouth parts adapted to sucking blood and legs adapted to grasping hairs. The life span of the female is approximately 1 month, during which time she lays 7–10 eggs each day, cementing them firmly to the base of a host hair. The eggs, commonly called nits, are oval lidded capsules that hatch in 8 days, releasing nymphs that require another 8 days to mature. After hatching, egg cases become white and more visible. Adults feed voraciously both on the scalp and adjacent areas of the face and neck.
Most lice infestations are asymptomatic; some children can harbor a surprisingly large colony of head lice. Itching of the scalp, neck, and ears may occur as an allergic reaction to lice saliva. Persistent or recurrent pyoderma about the neck and ears should always alert the examiner. Cervical and nuchal lymph nodes are often enlarged, and febrile episodes associated with secondary staphylococcal infection may occur.
Inspection using a fine-toothed nit comb is more efficient and effective for detecting lice and nits than a visual examination. Treatments include topical insecticides, such as permethrin, pyrethrin, and malathion. Additional treatments are wet combing and oral therapies (Figure 10).

Leprosy
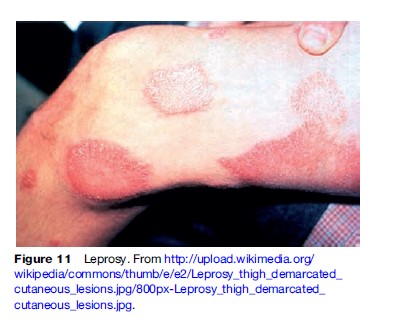
Hansen’s disease, also known as leprosy, is one of the oldest infections known to mankind and is still prevalent in the Indian subcontinent, Asia, and South America. Though primarily a disease of the developing countries, the significant disability associated with it makes it a disease of international importance. Leprosy has been divided into a spectrum based on its immunologic status. Patients with good immune responses may have tuberculoid leprosy and patients at the other spectrum are lepromatous and can harbor millions of bacilli in their nasal secretions.
It is caused by Mycobacterium leprae, which has an affinity to peripheral nerves, nasal mucosa and other cooler areas of the body. Its slow involvement of these structures is responsible for the sensory loss associated with the disease. The clinical characteristics are hypopigmented patches over the body or face associated with loss of sensation and adjacent nerve involvement. Progress toward the lepromatous spectrum can lead to formations of papules and nodules on the skin along with slow involvement of most of the organ systems.
The treatment consists of paucibacillary treatment for 6 months or multibacillary treatment for 1 year. The drugs used for treatment are dapsone, clofazimine, and rifampin, which are stored in multidrug packs and distributed freely for continual use. The greatest stigma associated with the disease are the hand and limb deformities that occur due to constant trauma to the peripheries (Figure 11).
Bibliography:
- Guldbakke KK and Khachemoune A (2007) Etiology, classification, and treatment of urticaria. Cutis 79(1): 41–49.
- Hanifin JM and Reed ML (2007) A population-based survey of eczema prevalence in the United States. Dermatitis 18(2): 82–91.
- Lipke MM (2006) An armamentarium of wart treatments. Clinical Medicine and Research 4(4): 273–293.
- Lowes MA, Bowcock AM, and Krueger JG (2007) Pathogenesis and therapy of psoriasis. Nature 445(7130): 866–873.
- Richardus JH (2007) Dermatologist. Treating leprosy. Leprosy Review 78(1): 56.
- Robles DT and Berg D (2007) Abnormal wound healing: keloids. Clinical Dermatology 25(1): 26–32.
- Sehgal VN and Srivastava G (2006) Vitiligo: Auto-immunity and immune responses. International Journal of Dermatology 45(5): 583–590.
- van Zuuren EJ, Gupta AK, Gover MD, Graber M, and Hollis S (2006) Systematic review of rosacea treatments. Journal of the American Academy of Dermatology 56(1): 107–115.
- Voskas D, Jones N, Van Slyke P, et al. (2005) A cyclosporine-sensitive psoriasis-like disease produced in Tie2 transgenic mice. American Journal of Pathology 166(3): 843–855.
- Wasserman D, Guzman-Sanchez DA, Scott K, and McMichael A (2007) Alopecia areata. International Journal of Dermatology 46(2): 121–131.
- Yosipovitch G, Tang M, Dawn AG, et al. (2007) Study of psychological stress, sebum production and acne vulgaris in adolescents. Acta Dermato-Venereologica 87(2): 135–139.
See also:
Free research papers are not written to satisfy your specific instructions. You can use our professional writing services to buy a custom research paper on any topic and get your high quality paper at affordable price.








